Primary care payment models are crucial in reshaping the landscape of healthcare reimbursement in the United States, especially amidst the primary care crisis that threatens to overwhelm a dwindling number of clinicians. As demand for primary care skyrockets, innovative strategies such as the prospective payment model are being explored to ensure that healthcare providers can deliver quality care efficiently. One promising approach to this challenge is the establishment of accountable care organizations (ACOs), which aim to bend the cost curve while enhancing patient outcomes through collaborative care efforts. By incentivizing preventive measures and reducing hospital visits, these models present an opportunity for significant medical cost savings and improved healthcare access for patients. Ultimately, the evolution of primary care payment models could provide a much-needed solution to the funding inadequacies that plague this vital sector of the healthcare system.
In the realm of healthcare financing, innovative compensation methods for primary care services are garnering attention as potential solutions for current systemic issues. These payment strategies, often encapsulated in terms like value-based care and capitated payment systems, are being tested to alleviate the pressures faced by providers in delivering essential medical services. With the emergence of structures like accountable care organizations (ACOs), the focus shifts towards incentivizing physicians to prioritize quality over quantity, reducing unnecessary hospitalizations and improving patient wellness. The exploration of these alternative payment frameworks aims not only to keep costs manageable but also to enhance the overall patient experience in primary care settings. As the healthcare landscape continues to evolve, understanding these underlying compensation models and their impact on clinician sustainability is more important than ever.
Understanding the Primary Care Crisis in America
The primary care system in the United States is facing a multifaceted crisis that demands urgent attention. With a skyrocketing demand for healthcare services and a dwindling number of primary care physicians, patients are often left waiting for appointments and struggling to receive timely care. Factors such as increasing patient volumes and the corporate ownership of practices contribute to a system that devalues the essential role of primary care providers. The emphasis on specialists and revenue-driven models has created a disparity in how services are reimbursed, causing primary care to be undervalued and underfunded.
Moreover, the influx of medical knowledge and the complexity of patient needs further complicate the landscape. Primary care physicians are tasked with managing more information than ever, yet their reimbursement rates remain disproportionately low compared to specialists. This crisis indicates a pressing need for innovative solutions that address the financing and structure of primary care, allowing physicians to focus on preventative care rather than being pressured by high patient loads. Enhancing primary care systems is not just about increasing reimbursement; it’s about reconsidering the entire healthcare model to foster sustainability and improve patient outcomes.
The Role of Prospective Payment Models in Primary Care
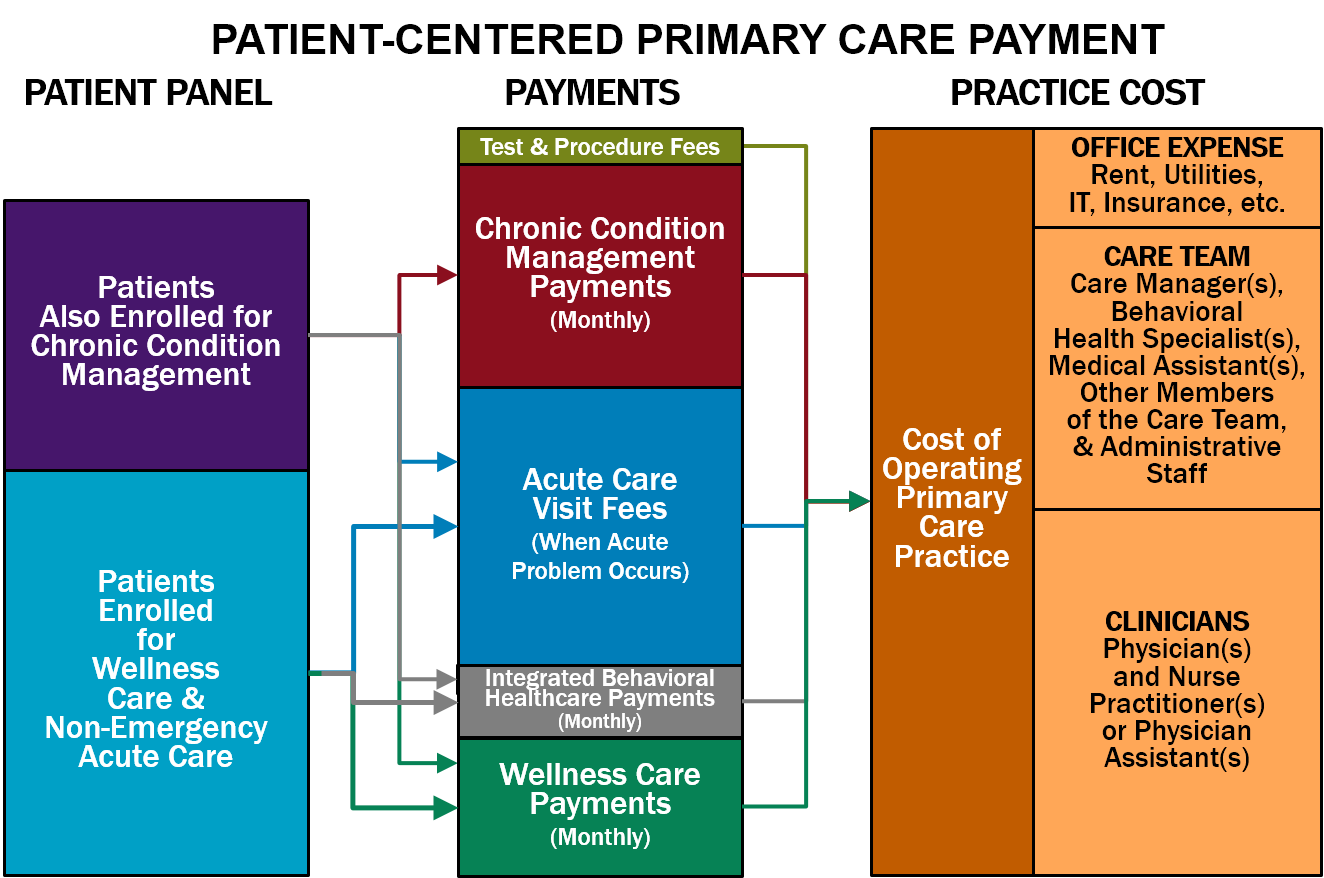
Prospective payment models are emerging as a revolutionary approach to healthcare reimbursement, particularly within primary care. Traditional models typically reimburse providers after services are delivered, often resulting in a focus on quantity over quality. In contrast, prospective payment systems, like ACO PC Flex, allocate funds to primary care practices before services are rendered, encouraging a proactive approach to patient health. By providing upfront payments based on regional averages, these models aim to incentivize practices to enhance their infrastructure and focus on preventative care, which is crucial in a system burdened by rising healthcare costs.
This shift toward prospective payment models aligns with the goal of reducing unnecessary hospital visits and preventing serious health complications. With financial backing before treatment begins, primary care providers can invest more time in patient counseling and health management, ultimately leading to better outcomes and potentially significant medical cost savings. As these models gain traction, they have the potential to reshape the landscape of healthcare reimbursement, prioritizing patient health over sheer volume of services performed, and addressing the primary care crisis head-on.
Innovations in Accountable Care Organizations (ACOs)
Accountable Care Organizations (ACOs) represent a groundbreaking shift in how primary care providers are reimbursed, emphasizing quality of care rather than the volume of services. The innovation of ACO PC Flex aims to improve care delivery by introducing shared savings models that reward physicians for keeping their patients healthy while managing healthcare costs. This model stands out by creating a financial framework where providers share in savings generated from efficient care management, thereby incentivizing a preventative approach instead of a reactive one.
As ACOs continue to evolve, the potential for these models to replace outdated reimbursement practices grows. By lowering costs and improving patient outcomes, ACOs could become a preferred structure for primary care across different insurance types. The key lies in demonstrating the effectiveness of these models in generating savings while maintaining high standards of care, which could inspire commercial insurers to adopt similar strategies. Ultimately, innovative ACO models have the potential to fortify primary care’s role in the broader healthcare system, benefiting both patients and providers.
Financial Incentives: Changes Needed for Primary Care Providers
One of the primary challenges facing primary care providers is the financial incentive structure currently in place. For decades, the healthcare reimbursement model has favored specialists with higher payment rates, leaving primary care practitioners struggling to make ends meet. This discrepancy leads to fewer clinicians entering primary care fields and a lack of investment in preventive care services, which are crucial for reducing overall healthcare costs. Adjusting the reimbursement framework to elevate primary care payment models is essential in addressing these issues.
Implementing changes that would rebalance the current fee schedules—essentially lowering specialist payments to increase those for primary care—could incentivize a new wave of healthcare professionals to enter primary care roles. Moreover, adequate remuneration for primary care services ensures that physicians can provide comprehensive, quality care to their patients. If the healthcare system prioritizes primary care as a foundational component, they will likely see significant improvements in health outcomes and efficiency across the board.
Potential Impact of ACO PC Flex on Medicare and Beyond
The introduction of ACO PC Flex has significant implications for Medicare patients and could serve as a model for broader healthcare reform. By employing a prospective payment system, this initiative offers a fresh approach to funding primary care, allowing providers to focus on preventative measures and chronic disease management. If successful, the outcomes observed in Medicare could catalyze a ripple effect where private insurers adapt similar payment structures, thereby improving accessibility and quality of care for all patients.
This model not only holds promise for Medicare enrollees but also emphasizes the need for increased funding for primary care in Medicaid, which serves a significant population of low-income patients with complex needs. Enhanced reimbursement rates would encourage more providers to serve Medicaid patients, ultimately improving health equity in the system. Should ACO PC Flex demonstrate effectiveness in reducing hospitalizations and overall healthcare costs, it could pave the way for a comprehensive overhaul of how the entire healthcare sector approaches primary care financing.
Challenges of Implementing New Reimbursement Models
Despite the promising nature of new reimbursement models like ACO PC Flex, challenges remain in their implementation across various healthcare settings. One significant hurdle is the resistance from existing power structures within the healthcare industry, where specialists have historically held a majority of influence in billing and reimbursement practices. The established norms favoring episodic and service-driven care conflict with the goals of integrated, patient-centered approaches that prospective payment models strive to establish.
Moreover, transitioning to new models requires education and support for primary care providers who may be unfamiliar with these systems. Ensuring that physicians understand the benefits and operational aspects of ACOs is crucial for successful implementation. Continuous evaluation and adaptation will also be necessary to measure outcomes and address any barriers to effective care delivery. Overcoming these obstacles will be essential to realize the full potential of these innovative payment models and significantly improve primary care overall.
The Future of Primary Care: A Look Ahead
As the healthcare landscape continues to evolve, the response to the primary care crisis must also adapt to the changing needs of patients and providers. Innovations like ACO PC Flex reflect a growing recognition of the importance of primary care in achieving better health outcomes and controlling costs. Looking ahead, it is vital that stakeholders in the healthcare system recognize the significance of investment in primary care, both in terms of financial resources and supportive policies.
The future may see a more integrated healthcare model where primary care is prioritized, paving the way for substantial reforms that redistribute funds to support primary care practices. By committing to proactive health management and preventive care, the healthcare system can not only reduce unnecessary expenditures but also foster healthier populations. Ongoing advocacy and research will be critical in shaping this future and ensuring that primary care receives the support it desperately needs.
Addressing the Inequality in Primary Care Financing
The stark contrast in funding between primary care and specialty services highlights a significant issue: healthcare inequality. Historically, primary care has been viewed as less lucrative compared to specialty fields, leading to a lack of investment that critically undermines the sector’s ability to meet growing patient demands. This disparity not only affects the financial viability of primary care practices but also limits patient access to essential services that could enhance health outcomes.
To address this inequality, efforts must focus on restructuring healthcare reimbursement practices, ensuring that primary care providers are adequately compensated for their essential role. Advocating for policies that value preventive care and holistic patient management will be critical. Solutions might include increasing funding through innovative models such as ACO PC Flex, which could realign incentives and establish a more equitable system. By confronting these disparities head-on, we can work to create a healthcare environment that treats primary care as a cornerstone of effective healthcare delivery.
Promoting Preventative Care Through Incentives
Incentivizing preventative care is fundamental to the success of modern healthcare systems, particularly in primary care. Models like ACO PC Flex underscore the importance of transitioning from a sick-care model to one that promotes health and wellness. By focusing on preventative measures and early interventions, healthcare providers can significantly reduce the incidence of costly acute and chronic illnesses. This requires a cultural shift within healthcare, where the value of preventive services is recognized and rewarded.
By implementing payment models that prioritize preventative care, healthcare systems can achieve better patient outcomes while simultaneously reducing costs. Providing physicians with the resources and incentives to focus on prevention will encourage a holistic approach to patient care. The shift towards a system that rewards health maintenance rather than solely treatment represents a crucial step in addressing the challenges currently faced by the primary care sector.
Frequently Asked Questions
What are primary care payment models and how do they impact healthcare reimbursement?
Primary care payment models refer to the various methods by which primary care providers are compensated for their services. These models, such as the prospective payment model and accountable care organizations (ACOs), are designed to improve healthcare reimbursement by incentivizing quality care while managing costs. Understanding these models is crucial in addressing the primary care crisis and ensuring that healthcare providers receive fair compensation for their vital services.
How do accountable care organizations (ACOs) fit into primary care payment models?
Accountable care organizations (ACOs) are an innovative primary care payment model aimed at improving healthcare delivery. ACOs incentivize healthcare providers to coordinate and provide high-quality care at lower costs. By focusing on preventive care and managing chronic conditions, ACOs can deliver medical cost savings, shifting the focus from volume of services to value of care. This model plays a pivotal role in addressing the challenges faced in primary care reimbursement.
What is a prospective payment model in primary care and why is it important?
The prospective payment model in primary care is a payment system where healthcare providers receive a set payment before services are delivered, based on factors such as average costs in the area. This model is important because it encourages primary care providers to focus on preventive care, ultimately reducing hospital visits and ensuring better health outcomes for patients. By increasing the overall investment in primary care, it addresses the financial challenges within the healthcare system.
How does the primary care crisis affect healthcare reimbursement models?
The primary care crisis, characterized by physician shortages and increasing demand for services, directly impacts healthcare reimbursement models. Insufficient funding for primary care leads to low reimbursement rates, making it difficult for providers to offer the necessary services. Innovative payment models like ACOs and prospective payments aim to mitigate this crisis by increasing the financial support for primary care, thus ensuring better quality care and lower costs for patients.
What benefits do prospective payment models bring to primary care providers?
Prospective payment models provide several benefits to primary care providers, including improved financial stability and incentives for preventive care. By receiving upfront payments tailored to patient demographics, providers can focus more on health outcomes and less on the volume of patients seen. This model addresses the historical financial disadvantage primary care has faced compared to specialists, promoting a more sustainable practice environment.
Can primary care payment models lead to medical cost savings?
Yes, effective primary care payment models, such as ACOs and prospective payments, can lead to significant medical cost savings. By incentivizing preventive care and reducing hospitalizations, these models help lower overall healthcare expenses while improving patient outcomes. Investing in primary care through innovative payment structures can ultimately reduce costs for both providers and patients in the healthcare system.
How might changes in primary care payment models affect patient care?
Changes in primary care payment models, like the introduction of ACOs and prospective payments, have the potential to enhance patient care. By focusing on quality over quantity, these models encourage primary care providers to spend more time on patient counseling and preventive measures. As a result, patients can expect improved access to care, better management of chronic conditions, and a more holistic approach to their health.
What role do healthcare reimbursement innovations play in solving the primary care crisis?
Innovations in healthcare reimbursement, such as new primary care payment models, play a crucial role in addressing the primary care crisis. By restructuring how providers are compensated, these models can ensure that primary care is adequately funded, allowing for better patient care and more resources for preventive services. Implementing such innovations will be key to reversing current trends and improving overall healthcare outcomes.
| Key Points |
|---|
| Primary care in the U.S. faces a crisis due to rising demand and a shortage of doctors. |
| The ACO PC Flex initiative aims to increase primary care spending and improve care delivery through upfront payments and incentives. |
| Current primary care is undervalued compared to specialists, leading to low reimbursement rates. |
| Accountable Care Organizations (ACOs) incentivize high-quality, lower-cost care through shared savings. |
| The prospective payment model of ACO PC Flex is a significant increase in payments for primary care. |
| If successful, ACO PC Flex could influence reimbursement models for non-Medicare populations. |
Summary
Primary care payment models are crucial in addressing the ongoing crisis in primary care, particularly in the United States. The introduction of innovative models like ACO PC Flex can potentially reshape how primary care is financed and delivered. By focusing on prospective payments and encouraging preventative care, these models aim to enhance patient outcomes while alleviating the financial pressures faced by primary care providers. The hope is that such initiatives not only improve care quality but also create a sustainable funding approach for a sector that has been historically undervalued.